The exhausting cycle that makes you overeat and keeps you away from energizing and sustainable eating
Do you overeat? Have you ever over-eaten? Have you ever felt a loss of control with your food intake? I think most of us have. From plates piled high at Thanksgiving Dinner to over-doing it on the holiday baking, we have all had meals and days when we have eaten more than what feels comfortable in our body. For some of us, it stops here. For others of us, this results in a soul-sucking cycle of restrict – overeat. You are not alone.
Trigger warning – the following post has blatant diet and weight talk as it explores over-eating. If you or someone you know if struggling with their eating or relationship with food, or has a suspected eating disorder, please contact a regulated health professional or visit http://nedic.ca/
What causes overeating?
There are many causes of overeating. The root of overeating is not your lack of self-control or will-power. Overeating can be caused by a metabolic adaptation to dieting. It can also be the result of chronic dieting, fuelled by resisting the change in our midlife bodies. One of the biggest predictors of over-eating is dietary restriction. If this information is a shock to you, maybe you need to read that again. One of the biggest predictors of you overeating is dietary restriction.
Many of us don’t see how we eat as restrictive. But as a dietitian working with clients in midlife, I see it all the time. Dietary restriction can take sneaky forms.
Here are a few ways diet restriction can look:
- Hoarding or controlling your food intake during the day (which is often followed by later day overeating).
- Describing your intake as “good” during the day, but then you find that you overeat in the late afternoon or evenings.
- Staying within a calorie “budget” while ignoring your body’s signals that it needs more fuel.
- Restricting your access to some foods, often based on categorizing foods as “good” vs “bad”, or “healthy” vs “unhealthy”.
- Applying “rules” to your eating, while disregarding evidence that said “rules” are not helpful to you.
- Changing your food intake after being triggered by someone else’s “approach” to what they have done to shrink their body.
- Limiting your food intake after being triggered by someone else’s well-meaning but totally unhelpful comment about how your body has changed.
Dietary changes fuelled in the spirit of restriction and control are unlikely to be sustainable or successful for you in the long-term. While most of us can do these “things” short-term, they are unlikely to be successful in the long-term (95-98% of people regain their lost weight after 2-5 years). And these restrictive dietary changes keep us stuck in a never-ending spiral of restrict-overeat while we chase the smaller body unicorn.
The restrict-overeat cycle that is more infectious than Covid
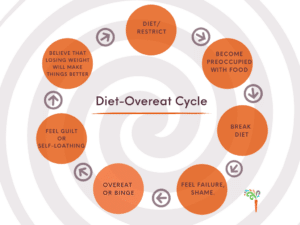
Have a look at the diagram below, called the “restrict-overeat cycle”. It is also called the “diet-overeat” or “eat-repent-repeat cycle”.
Let me walk you through this restrict-overeat cycle:
Diet/restriction – any diet or lifestyle action that is engaged in to manipulate your body into weight loss.
Become preoccupied with food – if you are manipulating your food intake with the hope of weight loss, you are likely to be thinking about everything that touches your lips. You may be counting calories or tracking your food intake. These activities can result in preoccupation with food and drink.
Break the diet – eventually, our body’s hormonal and survival mechanisms are turned on so strong within our bodies, the force is not resistible and we break our diet.
Feel failure or shame – We had set out to eat better. We thought we could control our actions with food. We are fed messages that if you want something badly enough, you can make changes even if they are tough. We are fed stories and anecdotes of someone else’s success, which initially might be inspiring, but that end up alienating us because it fuels the story that there must be someone wrong with me. Feeling like a failure or shame is an extremely uncomfortable emotion that is difficult to be with. Since we have already fXXked up, we may as well keep going and eat whatever we want.
Overeat – We may overeat on just one food or on several different foods. Afterall, we have already blown it. “I may as well just eat…..”. For some of us, we may feel a loss of control of our eating, like a ball rolling down the hill, which would be more like a binge.
Feel guilt or self-loathing – After overeating or binging, we often feel terrible. We feel physically uncomfortable for having over-eaten. Our bellies may hurt. We feel demoralized and alienated. We may begin in compare and despair, especially with people who may appear to have their food and diet “all together” (note: never judge a book by its cover. You have *no idea* what peoples true eating habits are behind what we observe publicly). We worry that this episode of over-eating is going to cause weight gain. Depending on how frequent this cycle occurs, it may have resulted in our body weight changing.
We believe that following stricter rules or guidelines, going on a diet or losing weight will make things better for us…after all, we feel that we cannot control what we eat. We believe we need more guidance. We need more control. And so the cycle continues.
Our culture makes energized & enjoyable eating difficult
Become aware of the culture in which you marinate
This restrict-overeat cycle is more infectious than Covid and is fuelled by the (toxic) culture in which we all live.
There are several aspects of our culture that make eating difficult:
The pressure to change our bodies – The culture where we are bombarded with messages of how we need to change our bodies to be better. The culture that glorifies smaller bodies, regardless of how they are created, and shames larger bodies, despite natural diversity in body size and shape.
The social comparison of food, eating, dieting and bodies that people do with each other, which also results in well-meaning but unhelpful comments and glorifications we do of each other. “Your so good with your diet”. “Have you lost weight? You look amazing.”
The pictures people post of their dieted bodies on social media, which invites the above comments.
Or the comments and judgements made about people behind their back. “Look at that person. They have gained weight”. Or “they have really let themselves go.”
Because we all marinate in this culture, we may not even be aware that this culture is the problem.
The presence of highly palatable foods – Food is everywhere in our environment. We don’t need to go far without seeing cues to remind us that we *might* be hungry. Highly palatable foods include sweet or salty snack foods. These foods are designed to tasty really good and to make you want more. These kinds of foods may be difficult to satiate with (although with mindful eating skills, we can notice when we have had enough – but most of us don’t use these skills).
The stress and relentless pressure we experience in our lives – Who doesn’t feel stressed or overly extended? The grief and trauma from the last few years hasn’t been easy on anyone. It has been worse for some of us. The hormonal changes we experience with stress, plus the learned soothing of stress with food often result in reaching for foods for which we have developed learned associations that eating this food makes us feel better. This repeated experience results in the formation of a habit loop of eating in response to stress or difficult emotions. And while we all do this from time to time, if this is our only stress management soothing strategy, this can be troublesome.
What is your experience with this restrict-overeat cycle?
This week, I’d invite you to think about whether you can see yourself in this cycle. And I’d like to plant the seed that you can focus on your health without focusing on restrictions or on your weight. Instead of working to control or manipulate your body, focus on connecting with and fuelling your body, while caring for the body you have *right now*. Connected eating creates embodied change that is energizing.
If you need help with getting off this cycle, please reach out to myself, or a professional with experience in supporting people with difficult relationships with food.
References:
Brewer JA, Ruf A, Beccia AL, et al. Can Mindfulness Address Maladaptive Eating Behaviors? Why Traditional Diet Plans Fail and How New Mechanistic Insights May Lead to Novel Interventions. Front Psychol. 2018;9:1418. Published 2018 Sep 10. doi:10.3389/fpsyg.2018.01418 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6139346/
Christopher L Melby 1, Hunter L Paris 2, Rebecca M Foright 3, James Peth 4 Attenuating the Biologic Drive for Weight Regain Following Weight Loss: Must What Goes Down Always Go Back Up? Nutrients 2017 May 6;9(5):468. doi: 10.3390/nu9050468. https://pubmed.ncbi.nlm.nih.gov/28481261/
Doucet E, McInis K, Mahmoodianfard S. Compensation in response to energy deficits induced by exercise or diet. Obesity Reviews 2018; December 19(Suppl 1): 36-46. https://www.ncbi.nlm.nih.gov/pubmed/30511511
J Polivy 1 Psychological consequences of food restriction. J Am Diet Assoc. 1996 Jun;96(6):589-92; quiz 593-4. https://pubmed.ncbi.nlm.nih.gov/8655907/
Burton AL, Abbott MJ. Processes and pathways to binge eating: development of an integrated cognitive and behavioural model of binge eating. J Eat Disord. 2019;7:18. Published 2019 Jun 7. doi:10.1186/s40337-019-0248-0 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6554957/
Mathes WF, Brownley KA, Mo X, Bulik CM. The biology of binge eating. Appetite. 2009;52(3):545-553. doi:10.1016/j.appet.2009.03.005 https://pubmed.ncbi.nlm.nih.gov/19501749/


Welcome to the Energize Nutrition blog, where we share evidence-based nutrition content, designed to empower people’s midlife. Take a look around to find information on feeling your best.
If you need more individualized support, reach out to set up a free discovery call with Kristyn Hall.

Battling chronic hunger, poor energy, or inflammation? Discover what this powerful ingredient is and why it might be the solution!