Can you increase GLP-1 naturally? A Guide for Appetite, Blood Sugars and Weight Concerns
Can you increase your GLP-1 hormone levels naturally—without medications? If you’ve wondered this, you’re not alone. In this blog, I’ll walk you through how your body already produces GLP-1, why it matters, and how to support GLP-1 production using food, habits, and gut health.
If you’ve heard of medications like Ozempic, Wegovy, or Mounjaro, then you’ve likely heard of GLP-1—a powerful and naturally-existing gut hormone that plays a major role in appetite control, blood sugar balance, and weight regulation.
What is GLP-1 and Why Does It Matter?
GLP-1 (glucagon-like peptide-1) is a hormone that is naturally secreted by specific cells in your gut shortly after you begin eating, typically within 10-15 minutes, with another peak 1-2 hours later (Huber et al 2024; Bondaruc et al 2016).
GLP-1 has several important functions (Mozzafariun et al 2025):
- Slows stomach emptying, helping you feel fuller longer
- Stimulates insulin release and helps lower blood sugar after meals
- Reduces appetite and food intake giving you a clear “stop eating” signal.
- Supports brain signals related to fullness and satiety, as well as reduced cravings.
- Reducing food cravings and “food noise”.
- May improve insulin sensitivity and fat metabolism
More recent evidence suggests that GLP-1 may also interact with the brain in ways that offer neuroprotective benefits. It has been shown to influence cognitive function and reduce brain inflammation in pre-clinical models (Huber et al., 2024).
In simple terms, GLP-1 helps regulate how much and when you eat, as well as how your body processes food—especially carbohydrates (Bodnaruc et al 2016; Miguens-Gomez et al 2021). GLP-1 is something that our bodies naturally produce and is stimulated by dietary intake.
But sometimes this GLP-1 system does not always work well. Like all aspects of being human, there is diversity in our GLP-1 system, depending on our metabolic health profile (Huber et al, 2024).
GLP-1 secretion may be impaired in individuals with metabolic health concerns like insulin resistance, or type 2 diabetes. These individuals often show blunted GLP-1 responses after meals, suggesting that improving baseline metabolic health can restore more robust GLP-1 signaling over time (Huber et al., 2024).
This finding highlights that the same dietary and lifestyle interventions that promote natural GLP-1 release, discussed more below, can also help correct the underlying issues that impair GLP-1 in the first place (Huber et al, 2024).
The Challenge: Why Not Just Use Medications to Increase GLP-1?
GLP-1 receptor agonists (like Ozempic, Wegovy and Mounjaro) are medications that mimic the effects of this naturally existing hormone, often resulting in significant appetite reduction and reduced cravings.
In a recent blog post, I wrote about How to eat if you take a GLP-1 Medication, where I outlined:
- what GLP-1 medications are
- how these medications work
- why GLP-1 Medications are gaining attention
- 6 key nutrition concerns for GLP-1 users
- GLP-1s and “food noise”, plus strategies to reduce food noise (regardless of GLP-1 use)
- What happens when I stop taking GLP-1s.
So why wouldn’t we just use medications to increase GLP-1 production?
For many reasons. These medications aren’t always accessible to people who may benefit from them:
- They are expensive (hundreds of dollars each month) and not always covered by insurance.
- Some people experience unpleasant side effects (e.g., nausea, constipation) that do not resolve over time, preventing its continued use.
- Others prefer not to use medications long-term (12% of US adults have used GLP-1 medications in the past, Mozafariun et al, 2025).
Whether due to cost, availability, tolerability or personal choice, GLP-1 medications are not always accessible to people who may benefit from them.
Fortunately, that doesn’t mean you’re without options—your body already produces GLP-1, and you can support it naturally through key nutrition and lifestyle strategies.
GLP-1 released from diet & lifestyle strategies vs GLP-1 from medications
The key difference to note is that the GLP-1 released via diet and lifestyle strategies stays active in the blood for significantly less time than the GLP-1 released via medications.
Circulating GLP-1 from diet and lifestyle has a “half-life” of 1-2 minutes before being inactivated in our bodies (Mozafariun et al 2025; Miguens-Gomez et al, 2021; Bodnaruc et al 2016), compared to the GLP-1 medications with a “half-life” of 7 days.
A half-life is the amount of time it takes for half of something to disappear or decay. It indicates how long it takes for the body to process or break down that substance.
GLP-1 from dietary sources has a very short “half life” compared to GLP-1 half life from medications.
So while the effect of food-based GLP-1 stimulation may be much shorter-lived, it still supports meaningful improvements in appetite regulation, blood sugar balance, and overall metabolic health—especially when these dietary strategies are practiced consistently (not rigidly or militantly).
In addition to dietary and pharmaceutical influences, new research confirms that GLP-1 secretion is impacted by sex as well as many personal health factors, including glucose tolerance and overall metabolic health, body weight, microbiome composition, and even eating behaviour itself (Huber et al., 2024).
Importantly, these factors don’t just influence GLP-1—they are also influenced by GLP-1, especially its effects on metabolic function and appetite regulation. This means that improving GLP-1 through diet and lifestyle can create a feedback loop that may support long-term metabolic resilience (Huber et al 2024).
This makes dietary and behavioural strategies especially meaningful for individuals with impaired GLP-1 signalling, such as those with insulin resistance, obesity or type 2 diabetes. In fact, improving these underlying metabolic factors may help restore more effective GLP-1 release over time (Huber et al 2024).
So while we aren’t comparing apples to apples when comparing GLP-1 stimulated via diet versus a GLP-1 from medication, we also know that not everyone can take a GLP-1 medication. So what options exist for this group of people?
That is what this blog post is about.
The good news is that your body already makes GLP-1, and there are natural ways to support and enhance its production through diet and lifestyle, though as explained above, this is not a direct or equivalent comparison with medications due to the vast differences in the half-life length.
Let’s explore how you can support natural GLP-1 release with food, nutrients, lifestyle habits, and gut health.
7 Ways to Support Your Body’s Natural GLP-1—without Medication
1. Feed Your Gut Fiber-rich Carbohydrates
Your gut health plays a critical role in GLP-1 secretion, especially in the colon, where fermentation of undigested carbohydrates produces substances called short-chain fatty acids (SCFAs), like butyrate, propionate and acetate. These SCFAs not only nourishes colon cells and reduces inflammation, but also stimulates GLP-1 secretion via G-protein-coupled receptors. This creates a positive feedback loop: more fiber leads to more SCFA, which promotes more GLP-1, supporting blood sugar and appetite regulation (Mozafariun et al 2025; Bodnaruc et al, 2016; Sing et al, 2024). Proprionate directly boosts GLP-1 secretion from specific cells in the gut (Singh et al, 2024).
The best sources of fiber-rich carbohydrates include:
- Fermentable fiber from foods like oats, barley, lentils, beans, and root vegetables
- Resistant starches, found in cooled cooked potatoes, green bananas, and legumes
- Whole grains, especially high-fiber intact grains and minimally processed oats
- Psyllium fiber supplements.
Tip: Aim for at least 25–35g of fiber daily, with an emphasis on fermentable fibers.
2. Include Healthy Fats (Especially MUFAs and Omega-3s)
Not all fats are created equal.
We can classify fats by their chemical structure, with some having no double bonds (saturated fats), and some having at least one double bond (a mono-unsaturated fat) or more than one double bond (a polyunsaturated fat). An omega-3 fat is when this double bond is located at the third carbon position from the “methyl end”. 🤓
Research shows that a kind of fat called unsaturated fats, especially monounsaturated fats (MUFAs) and omega-3s, enhance GLP-1 secretion more effectively than saturated fats.
Best sources of fats to help release GLP-1s:
- Olive oil (a staple of the Mediterranean diet)
- Avocados
- Fatty fish (salmon, sardines, mackerel, arctic char, trout)
- Nuts and seeds (raw almonds, walnuts, pistachios, whole peanuts, flaxseeds, natural peanut butter, flax seeds, chia seeds, hemp hearts)
In fact, a diet high in olive oil increased GLP-1 levels, improved insulin sensitivity, and reduced weight gain in several studies (Bonaruc et al, 2016). A Mediterranean diet was found to result in higher GLP-1 release than a Western diet (Huber et al 2024).
3. Prioritize Protein (Especially at Breakfast)
Protein-rich food help us to feel full (Mozzafarian et al 2025; Miguens-Gomez et al, 2021; Bodnaruc et al 2016). In fact, protein is the most satiating macronutrient! Its digestion stimulates GLP-1 release. Several protein sources increase GLP-1 release (Miguens-Gomez et al 2021). Some protein-rich foods help to prevent the de-activation of GLP-1 (Miguens-Gomez 2021).
Including a variety of protein-rich food at each meal helps you stay full and gives you stable energy throughout the day.
Best sources:
- Dairy proteins like Greek yogurt, cottage cheese
- Chicken, turkey, lean beef, tofu
- Eggs
- Lentils, edamame, tempeh
- Protein-containing snacks like almonds, pistachios, and peanut butter (these foods are healthy fats that also include some protein in them).
👉 Try this: Start your day with a GLP-1 friendly breakfasts:
- oatmeal topped with Greek yogurt, nuts, berries
- scrambled eggs + black beans with fresh tomatoes in a whole grain wrap
- blueberry & avocado smoothie with soy milk and pasteurized egg whites.
Hungry for high-protein breakfast recipes?
Grab my free recipe pack here

4. Add Polyphenol-Rich Foods for Gut and Hormonal Health
Adding in foods rich in polyphenols helps to improve our gut and hormonal health (Miguens-Gomez et al, 2021; O-Connor 2025).
Polyphenols are plant compounds that feed your beneficial gut bacteria—including bacterial strains associated with increased GLP-1 production, like Akkermansia muciniphila. These bacteria also help strengthen your gut lining and reduce inflammation (O’Connor 2025).
Best polyphenol sources:
- Berries (blueberries, raspberries, blackberries)
- Dark leafy greens (spinach, kale)
- Artichokes, olives, onions
- Green tea, black tea, and coffee
- Dark chocolate and unrefined cocoa
- Spices like cinnamon, turmeric, ginger
5. Consider Probiotics and Prebiotic Foods
Healthy gut bacteria are a key link in the GLP-1 production chain. Certain probiotics may help support GLP-1 secretion indirectly by promoting better fermentation and SCFA production (Huber et al, 2024; O’Connor, 2025).
Probiotic supplements with strains like Akkermansia and Bifidobacteria are also being explored in GLP-1-related protocols (O’Connor, 2025).
You can also eat prebiotic foods to “feed” your healthy gut bacteria (O’Connor, 2025):
- Garlic, onions, leeks
- Asparagus, Jerusalem artichokes
- Bananas, oats, apples
6. Eat Slowly & Mindfully
You’ve heard that it takes time (~ 15-20 minutes) to feel full. Here is one reason why it helps to eat slowly and mindfully:
In our body, GLP-1 release happens in two waves (Bodnaruc et al 2016; Miguens-Gomez 2021):
- A fast, neural-based release within 10-15 minutes of eating
- A slower, nutrient-based release ~60 minutes after eating, especially when nutrients reach the lower GI tract,
Eating too quickly may short-circuit the gut-brain connection. Slow down and chew thoroughly to allow your vagal nerve (which senses fullness) to kick in and help regulate appetite.
When we wait too long to eat, it is normal to get voraciously hungry. When we get this hungry, we tend to eat fast and eat larger amounts than we otherwise would when we eat in a more consistent meal and snack pattern. We also tend to reach for food-like products that are fast, quick and easy.
The solution, for the most part, is to strengthen our meal pattern, fueling our body more regularly and consistently, but without grazing.
Newer research shows that GLP-1 secretion is not only a result of what we eat, but also how we eat. Eating behavior—including meal timing, food reward, satiety responsiveness, and even mindful eating—can impact the release and activity of GLP-1 (Huber et al 2024). This further supports the importance of behavioral strategies like eating slowly, tuning into hunger and fullness cues, and reducing ultra-processed food intake as part of a GLP-1-friendly lifestyle.
7. Space Out Meals to Allow Hormonal Recovery
GLP-1 levels gradually decrease after about 2 hours after a meal (Bodnaruc et al 2016). Eating too frequently (e.g., grazing) may blunt this hormonal rhythm.
A strategy is to eat balanced meals every 3–5 hours, where there are periods of fueling and then periods of “rest”, allowing time for your body to “rest and digest” as well as hormones to “reset”.
Sample Daily Eating Plan to Boost GLP-1
Here’s a snapshot of how to put this into practice:
| Meal | GLP-1 Friendly Ingredients |
| Breakfast | Oatmeal + Greek yogurt + blueberries + flax + cinnamon |
| Lunch | Edamame and barley salad + lemon olive oil dressing + arugula + pistachios + green tea |
| Snack | Apple slices with almond butter |
| Dinner | Salmon + roasted sweet potatoes + broccoli + avocado |
| After-dinner wind-down | Herbal tea + piece of dark chocolate (85% cocoa) |
The Role of Lifestyle and the Gut Microbiome
Beyond food, gut health is a key player in supporting natural GLP-1 production (Huber et al 2024; O’Connor 2025). Within the gut, a thick mucin layer and tight gut lining help protect against inflammation and metabolic dysfunction. Akkermansia bacteria help maintain gut barrier integrity and promote GLP-1 production. Butyrate, a SCFA from fiber fermentation, slows digestion and increases GLP-1 production (Huber et al, 2024; O’Connor 2025).
Emerging evidence highlights how GLP-1 not only influences appetite and insulin secretion but also reshapes the gut microbiome (Singh et al, 2024). For example, GLP-1 agonists have been shown to increase beneficial bacteria such as Bacteroides, Lactobacillus, and Bifidobacterium, while reducing inflammatory species with Enterobacteriaceae. These shifts help strengthen gut barrier integrity and reduce systemic inflammation, which are both key to improving insulin sensitivity and reducing appetite (Singh et al, 2024).
You may expect improvements in gut-driven GLP-1 production in ~90 days of consistent dietary and lifestyle change (O’Connor 2025).
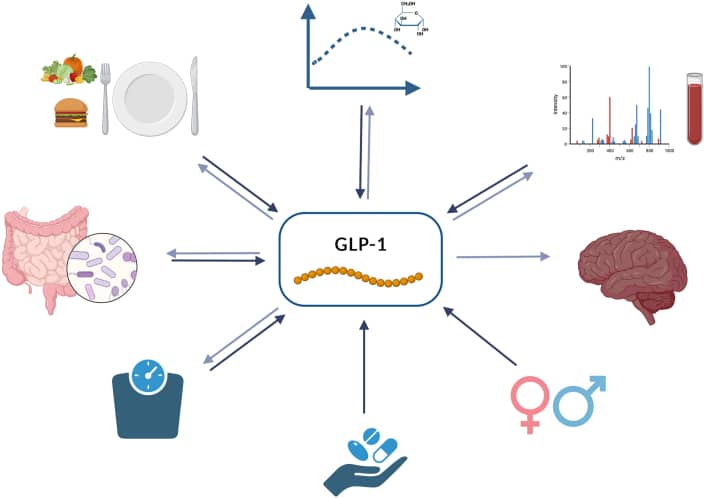
Huber et al (2024). included a figure showing the two-way influence between GLP-1 and metabolic/lifestyle factors. GLP-1 is both influenced by and exerts effects on variables like the microbiome, eating behaviour, glucose tolerance, metabolic profile, medication, sex and weight. GLP1 also affects these factors (except sex and medication). This two-way influence creates a dynamic loop where diet, microbiome, and behavior all play a role in modulating GLP-1 secretion.
GLP-1, Bile Acids and Fat Absorption
Recent studies show that GLP-1 agonists modulate bile acid metabolism by increasing the growth of gut bacteria that deconjugate bile acids. This leads to less fat being absorbed and more energy being burned, which may explain part of GLP-1’s effectiveness in supporting weight management (Singh et al, 2024).
The Gut-Brain Axis and Emotional Eating
GLP-1 impacts the gut-brain axis – an intricate communication system between the gut microbiota and brain – via neural, immune and hormonal signalling (Singh et al, 2024). Adiposity-related Inflammation weakens satiety signals and increases cravings. GLP-1 supports mental wellness by restoring microbial balance and improving satiety signalling, potentially reducing emotional eating and cravings (Singh et al, 2024).
Main factors influencing GLP-1 secretion
Huber et al (2024) included a figure showing the two-way influence between GLP-1 and metabolic/lifestyle factors. GLP-1 is both influenced by and exerts effects on variables like the microbiome, eating behaviour, glucose tolerance, metabolic profile, medication, sex and weight. GLP-1 also affects these factors (except sex and medication). This two-way influence creates a dynamic loop where diet, microbiome, and behaviour all play a role in modulating GLP-1 secretion.
A summary of the main factors influencing GLP-1 secretion is shown in the image below (Huber et al, 2024).
Source: This is an open access article under the CC BY-NC-ND license (http://creativecommons.org/licenses/by-nc-nd/4.0/). Need a bigger view of this image? Click here.
Bottom Line & Key Takeaways:
GLP-1 is a powerful hormone that your body already produces. However, GLP-1 from dietary sources has a very short “half life” compared to GLP-1 half life from medications.
You can support GLP-1 naturally through the foods that you add to your dietary pattern.
- Eat fiber-rich carbohydrates (especially fermentable fiber)
- Choose healthy fats, especially olive oil, nuts, seeds, foods rich in omega-3s
- Prioritize protein in every meal
- Feed your gut microbiome with polyphenols, prebiotics, and probiotics
- Supporting the growth of bacteria like Akkermansia mucinilphila and Bifidobacterium – both of which are linked to increased natural GLP-1 production – may offer another layer of support. Prebiotic-rich foods (like onions, garlic, oats, asparagus) and possibly targeted probitoics may be worth exploring when improving metabolic health.
- Eat slowly and mindfully, giving your body time to rest and digest between meals.
By focusing on your dietary pattern, gut health, and mindful habits, you can tap into your body’s own GLP-1 production to help support metabolic health, appetite regulation, and limit weight concerns.
Supporting your GLP-1 production naturally isn’t about perfection—it’s about nourishment, building consistency, and learning what works for your body. Small changes can have a big ripple effect on your energy, appetite, and health.
If you need help with creating diet and lifestyle change, a registered dietitian skilled in behaviour change strategies can help you.
References consulted in writing this post:
Alexandra M Bodnaruc 1, Denis Prud’homme 2, Rosanne Blanchet 3, Isabelle Giroux 4 Nutritional modulation of endogenous glucagon-like peptide-1 secretion: a review. Nutr Metab (Lond). 2016 Dec 9:13:92. Available from: https://pubmed.ncbi.nlm.nih.gov/27990172/
Hanna Huber 1, Alina Schieren 2, Jens Juul Holst 3, Marie-Christine Simon 4 Dietary impact on fasting and stimulated GLP-1 secretion in different metabolic conditions – a narrative review. Am J Clin Nutr. 2024 Mar;119(3):599-627
Alba Miguéns-Gómez # 1, Àngela Casanova-Martí # 1, M Teresa Blay 1, Ximena Terra 1, Raúl Beltrán-Debón 1, Esther Rodríguez-Gallego 1, Anna Ardévol 1, Montserrat Pinent 1. Glucagon-like peptide-1 regulation by food proteins and protein hydrolysates. Nutr Res Rev 2021 Dec;34(2):259-275. Available from: https://pubmed.ncbi.nlm.nih.gov/33461642/
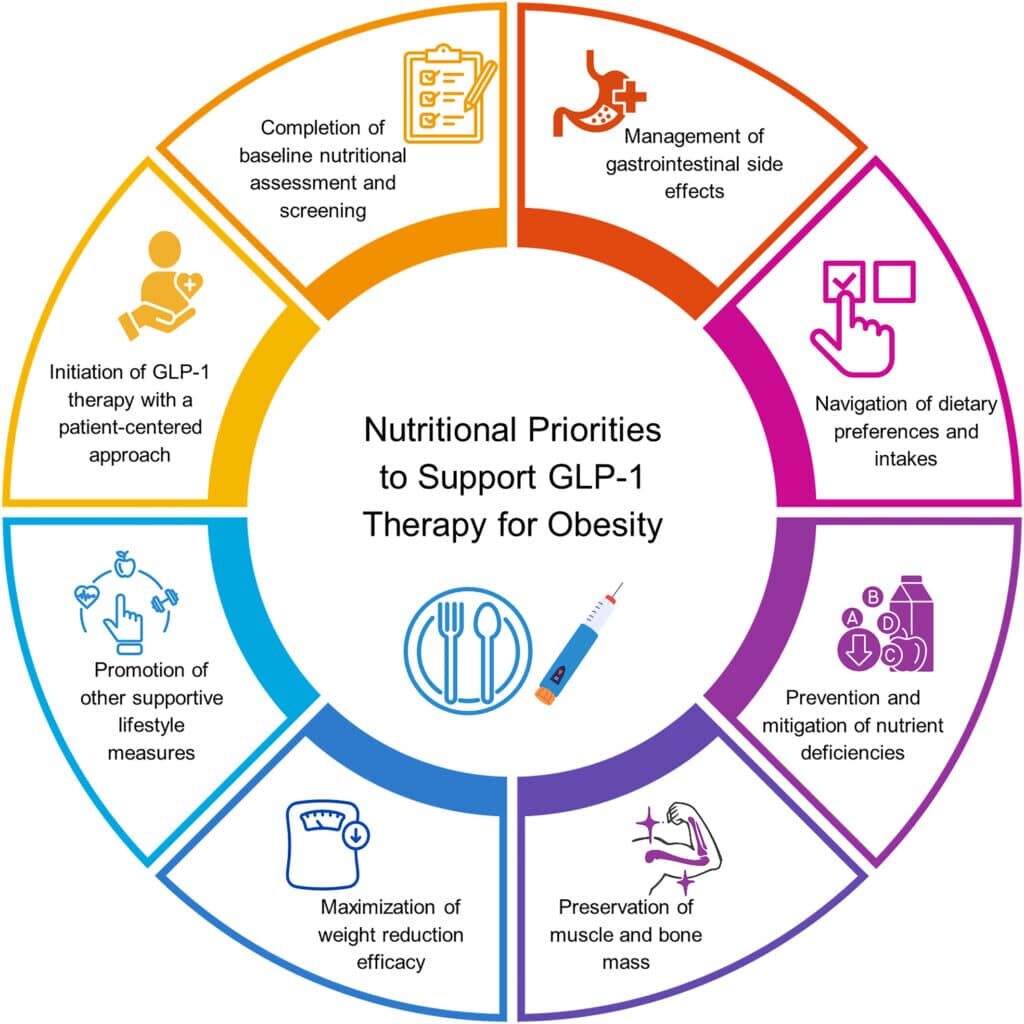
Dariush Mozaffarian 1, Monica Agarwal 2, Monica Aggarwal 3, Lydia Alexander 4, Caroline M Apovian 5, Shagun Bindlish 6, Jonathan Bonnet 7, W Scott Butsch 8, Sandra Christensen 9, Eugenia Gianos 10, Mahima Gulati 11, Alka Gupta 12 13, Debbie Horn 14, Ryan M Kane 15 16, Jasdeep Saluja 17, Deepa Sannidhi 18, Fatima Cody Stanford 19 20, Emily A Callahan 1. Nutritional priorities to support GLP-1 therapy for obesity: A joint Advisory from the American College of Lifestyle Medicine, the American Society for Nutrition, the Obesity Medicine Association, and The Obesity Society. Obesity (Silver Spring). 2025 May 30. doi: 10.1002/oby.24336. Online ahead of print. Available from: https://pubmed.ncbi.nlm.nih.gov/40445127/ and https://ajcn.nutrition.org/action/showPdf?pii=S0002-9165%2825%2900240-0
O’Connor Christina. Optimizing GLP1 hormone production through the lens of the gut microbiome. Webinar, June 2025. Available from: https://vimeo.com/1077750669
Singh, K., Aulakh, S. K., Nijjar, G., et al. (2024). Rebalancing the Gut: Glucagon-Like Peptide-1 Agonists as a Strategy for Obesity and Metabolic Health. Cureus, 16(7). https://doi.org/10.7759/cureus.64738


Welcome to the Energize Nutrition blog, where we share evidence-based nutrition content, designed to empower people’s midlife. Take a look around to find information on feeling your best.
If you need more individualized support, reach out to set up a free discovery call with Kristyn Hall.

Battling chronic hunger, poor energy, or inflammation? Discover what this powerful ingredient is and why it might be the solution!